Vets ask for farmers’ help with distressing teat condition
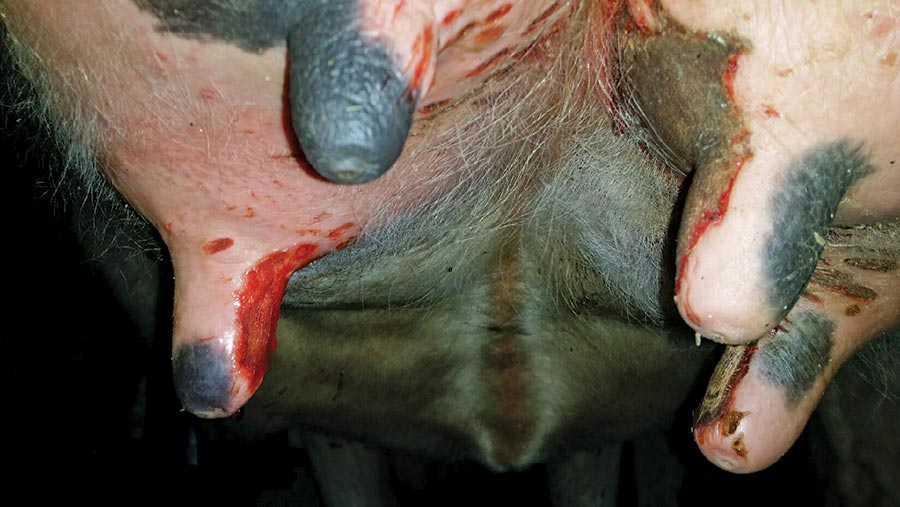
Vets are calling on farms to demystify a painful teat condition that can lead to stricken cows chewing off their own teats.
Ischaemic teat necrosis (ITN) is a costly condition mainly affecting first-calving heifers. A pea-sized scab on one udder can spread across all four quarters within 12-24 hours, making milking parlour vigilance critical in spotting ITN early.
While there have been studies into the disease, scientists are yet to find a cause and cure. Culling animals, often in early lactation, is the only option for a growing number of herds.
See also: Video: Herdsman’s tips on beating ischaemic teat necrosis
Worst-known culling levels have been as high as 25% of heifers on a 400-cow, robot-milked dairy for two consecutive years, although affected farms typically report one or two cases a year.
Similarities with digital dermatitis bacteria
- Pungent, fetid odour
- Moist stippled appearance (resembling other treponemal skin infections)
- Reports of treponemes isolated from ulcerative mammary dermatitis
- Results from vet observations
Most cases are seen in high-yielding Holstein-Friesians, but cases in 5,000-litre lactation herds, cross-bred and Jersey herds have been reported too.
First described in Vet Record by Gloucestershire vet Roger Blowey in 2004, the condition has since been shown to have global implications, with Mr Blowey at the time reporting a “considerable increase” in cases over the previous year.
The ailment is now known to be affecting farms across the length and breadth of the UK and has been linked to the same causal bacteria behind digital dermatitis lesions, according to Al Manning at the Royal Veterinary College.
Morbidity rates
“Morbidity is quite high. However, mortality from the disease appears to be low, but most cases are removed from the herd as, without udders, they are useless as a dairy cow,” he said.
“Geographically, it seems to be much more widespread than we initially thought. We have received emails from around the world, as far away as Uruguay, with a disease which appears to be similar.”
Along with researchers at Liverpool University, Mr Manning is keen to hear from as many farmers as possible to share accounts of ITN to help secure grants for research.
Farmers are urged to send in:
- Images of affected teats.
- Figures of cases and culls.
- Details about novel treatments and coping with the condition.
- Information about the system –bedding, milking intensity, parlour routine.
What to look out for
“It usually starts with a dry, scabby lesion at the base of the teat, most commonly in heifers,” Mr Manning said. “It progresses down the teat and can spread to the udder tissue.
“There is no formation of warts or blisters like in some other teat diseases. Ultimately, it is so painful that affected animals have been reported to chew their own teats off.
“Affected herds usually have only a handful of cases and currently very little is known about the disease.”
Preliminary findings of a Liverpool University study
- Most common in first lactation heifers in early lactation.
- Farms that suffered with ITN had a variety of bedding, teat liners, milking techniques, milking intensity and systems (housed and grazing).
- 80-95% of cases were in freshly calved heifers, with very few cases in cows.
- It is resistant to a wide range of treatments, from injectable steroids and antibiotics, to antibiotics sprays, Stockholm tar, teat dip, udder salve, topical iodine, copper sulphate solution, hydrochlorite and fusidic acid.
Cure rate facts
- Cure rates are low. A study found eight of 43 cases were curable, the rest had to be culled.
- Must be identified within 24 hours.
- Nsaids, topical salves and vasolidators (increase bloodflow by relaxing smooth-muscle cells) have been shown to lessen the condition if caught early.
If you have ITN on your unit, you can send case information, details of herd losses and pictures of affected udders to Al Manning at the RVC (amanning@rvc.ac.uk), which is trying to identify risk factors for the disease and test treatments. At Liverpool University, Simon Clegg (s.r.clegg@liverpool.ac.uk) will soon be leading an AHDB- and government-funded research programme.
